Does Snoring and Obstructive Sleep Apnea (OSA) damage Upper Airway Motor nerves?
Snoring is a form of sleep disordered breathing, but far from just being a benign nuisance to the bedpartner, we know of its association with various other diseases especially stroke. But is it possible that snoring can become a viscous cycle upon itself?
Many clinical studies have now identified nerve dysfunction and injury in adults with Obstructive Sleep Apnea (OSA). The nerves of sensation have reduced activity (called action potentials) and show reduced power (amplitude) in individuals with OSA which may be corrected in some cases.
This means that people who snore damage the nerve supply to their airway which may make the situation worse.( A vicious cycle).
So this indicates that OSA may cause effects which worsen the disease itself. It also indicates that early intervention likely outweighs the “watch and wait approach” as the disorder worsens. In other words, if you don’t know its damaging itself, you wait until it does – which doesn’t make much sense.
Perhaps our largest concern should be the lack of awareness shown by many physicians who maintain this potentially devastating disease state in their patients unaware of its inexorable progress.
We already know that snoring is not benign, we know that there is a strong association between snoring and stroke, but here’s another reason to prevent snoring.
Electrical studies of muscles (EMG) especially the study of the palatopharyngeus muscle shows long poly phasic potentials with decreased amplitude in patients with OSA, (confused and weakened power in the nerve) and histologically, under the microscope, identified loss of the structural coat of the nerve (demyelination) in the tissues of the palate.
There is an association of this damage with the kind of oxygen lack that occurs on and off during OSA and snoring. (The severity of these peripheral nerve dysfunction correlates with Chronic Intermittent Hypoxia (CIH)oxygen desaturation in OSA. Long term exposure to CIH impairs hypoglossal motor neurons.)
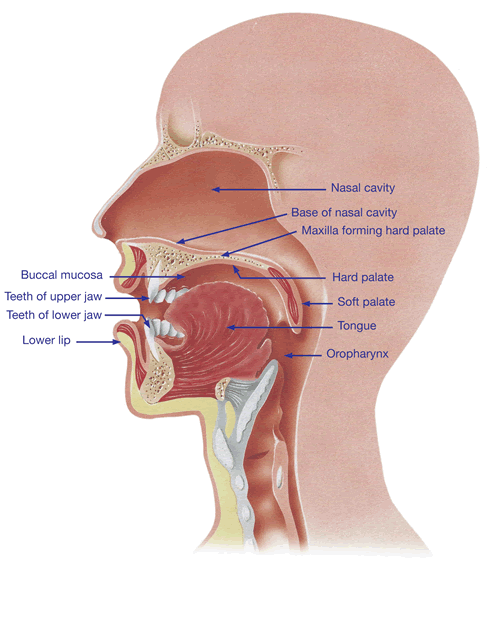
As well as being suspected of mechanical damage to the carotid artery in the neck from vibration caused by snoring, it may conceivably be responsible for damaging upper airway nerves and muscles from mechanical and chemical means too.
Available information suggests that inflammatory cell infiltration and denervation changes affect not only the upper airway muscle of patients with OSA, but also their upper airway surface tissues (mucosa).
This may have important implications for the ability to generate adequate muscular dilating forces during sleep, without which the airway may be more prone to collapse.
Clearly early diagnosis and adequate treatment is desperately needed in this often ignored yet potentially life-threatening disease. It is hoped that Primary care physicians will consider referral, management or treatment.
CLICK BELOW TO RECEIVE YOUR FREE “BETTER SLEEP” GUIDE
Good sleep is crucial to good health and longevity.
Dr. Stephen Bray 2019


